Playlist
Show Playlist
Hide Playlist
Hypertension: General Treatment
-
Slides Hypertension ChronicCare.pdf
-
Download Lecture Overview
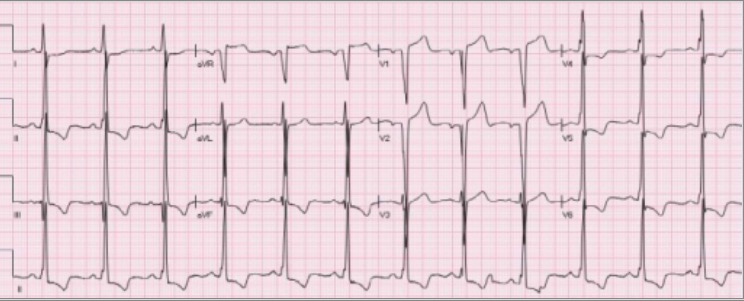
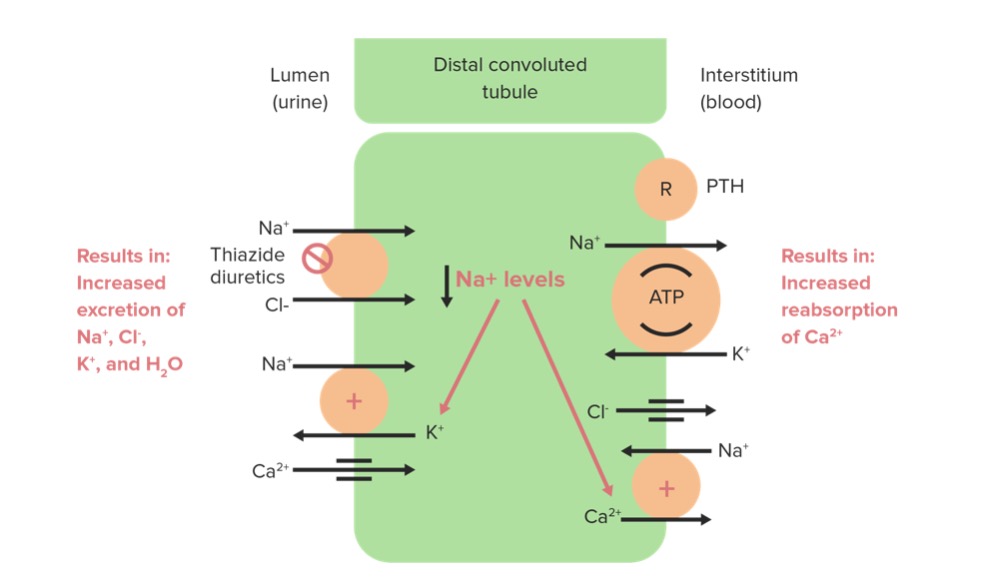
00:01 And what about secondary hypertension? When do you see that? I think a secondary hypertension, it's rare. 00:07 It's only up to 10% of cases of hypertension. 00:10 It’s probably less than that. 00:11 But especially, in a middle-aged adult, when they come in with a very high blood pressure, and particularly a blood pressure that’s not well controlled on initial therapy, you can consider some differential diagnosis. 00:23 Thyroid disease is very easy to test for and pretty common, but oftentimes it will also be associated with other symptoms and a pulse if they're hyperthyroid that's high. 00:33 So, therefore, you can ferret out that they have thyroid disease from other historical factors. 00:38 It’s rare when it’s just sitting there. 00:40 And the only symptom it's really causing is high blood pressure. 00:44 Hyperaldosteronism can be a problem. 00:46 Conn syndrome. 00:47 So, look for electrolyte abnormalities associated with that. 00:51 Renal artery stenosis is the most common cause of secondary hypertension. 00:55 And if it’s middle-aged adults, you're probably talking about acquired renal artery stenosis as opposed to congenital renal artery stenosis. 01:03 This – watch what their GFR, their glomerular filtration rate, is doing. 01:09 Watch their creatinine levels. 01:11 But it often needs analysis with something like either a CT or magnetic resonance angiography of the renal arteries. 01:20 And pheochromocytoma, we all worry about it. 01:22 It's actually incredibly rare. 01:24 And again, these patients usually have other symptoms – tremor, sweating and weight loss – that can give away the fact that they have this excess of catecholamines. 01:34 It's rare that it’s just – oh, the blood pressure is elevated by itself. 01:40 What do you to evaluate patients once they are diagnosed with hypertension? Everybody gets a baseline electrocardiogram, looking for things like left ventricular hypertrophy or prior cardiac damage, glucose level or an HbA1c, something to screen for diabetes, something to screen for hyperlipidemia, a check of their electrolytes along with their kidney function, as well as a hemoglobin level and urinalysis or a microalbumin creatinine ratio to check for the possibility of proteinuria and early kidney disease. 02:09 That's your baseline. 02:10 And these essentially should be repeated at least when we talk about the electrolytes, the urinalysis on an annual basis. 02:21 At least. At least on an annual basis. 02:24 Remember the lifestyle changes are still at the foundation for the treatment of hypertension. 02:30 And actually if you look at something like the dietary approaches to stop hypertension, that reduction on average with 11.5 over 5.5 points of mercury is really remarkable. 02:43 That's more powerful than most anti-hypertensive agents. 02:46 And, obviously, patients can do a DASH. 02:49 That’s going to yield other good things in terms of their cholesterol and their metabolism, their body weight. 02:55 So, there are side benefits to that diet that are really wonderful. 02:59 But that reduction in blood pressure values is outstanding. 03:04 Weight loss certainly promotes a lower blood pressure as well. 03:09 So, that's one of the benefits of, say, bariatric surgery. 03:12 A lot of patients are cured of hypertension, following the significant weight loss they experience with bariatric surgery. 03:19 But even following a good diet and exercise and losing 4 kilos can result in a significant reduction in blood pressure. 03:27 And exercise, as I mentioned, in and of itself can reduce blood pressure as well. 03:31 So, these are the keys. 03:33 And you can see that, if you put all of these things together, many patients wouldn't – could avoid medical therapy completely if they really embraced diet and exercise. 03:47 So, let’s return to our case. She has actually come back to clinic now. 03:51 And a repeat blood pressure, unfortunately, despite trying to do her lifestyle changes in the past two weeks, is 150/94. 03:58 Her pulse is 86 bpm. 04:00 So, now, what do you want to do? Do you want to allow six months for lifestyle changes to have an affect since she started them? Do you want to start a thiazide diuretic, start an alpha adrenergic blocker or start a beta blocker? Which one would you choose? I would go with a thiazide diuretic. 04:16 That is recommended as a first-line therapy by JNC 8. 04:20 So, here are the first-line treatments after lifestyle for hypertension. 04:25 And JNC 8 left this fairly open. 04:28 And again, these are only recommendations, but the recommendations are broad and catch most patients, I think. 04:34 Thiazide diuretics are a great option for patients. 04:39 One thing, whenever I prescribe a diuretic, is that I will ask them if they have any urinary issues. 04:45 Many older adults have overactive bladder or benign prostatic hypertrophy, and therefore, already may be struggling with genitourinary issues. 04:55 I don't want to exacerbate that by giving them a thiazide diuretic. 04:59 I would choose something else for those patients. 05:02 The other thing is prescribing a thiazide alone – watch closely for the potassium because thiazide promotes hypokalemia. 05:10 Whereas ACE inhibitors and ARBs, also considered a first-line agent, can promote hyperkalemia. 05:16 So, therefore, a combination of one of those agents with a thiazide is helpful in terms of maintaining normokalemia. 05:24 And calcium channel blockers have their own range of side effects, but one thing they don't do much is affect electrolytes. 05:31 It’s also worth noting that atenolol is not recommended by JNC 8. 05:34 It doesn't confer overall the same mortality benefit for cardiovascular disease that these other agents maintain.
About the Lecture
The lecture Hypertension: General Treatment by Charles Vega, MD is from the course Chronic Care. It contains the following chapters:
- Secondary Hypertension
- Initial Evaluation of Patients with HTN
- Treatment of HTN
Included Quiz Questions
Which of the following tests is NOT included in the initial evaluation of all patients with newly diagnosed hypertension?
- Echocardiography
- Fasting glucose
- Lipid profile
- Urinalysis
- Electrocardiogram
In patients with hypertension, which of the following lifestyle interventions leads to the most significant drop in systolic blood pressure?
- Healthy diet
- Weight loss
- Regular exercise
- Smoking cessation
- Alcohol reduction
What is the average reduction in systolic blood pressure for every 1 kg reduction in body weight?
- 1 mm Hg
- 0.5 mm Hg
- 2 mm Hg
- 5 mm Hg
- 10 mm Hg
Which of the following is the most appropriate diagnostic evaluation in patients who are suspected of having secondary hypertension and do not have primary kidney disease, primary aldosteronism, or pheochromocytoma?
- Evaluation for renovascular hypertension
- Cardiac angiography
- Cardiac stress test
- Renal biopsy
- No further evaluation is required.
Which of the following antihypertensive medications is most likely to cause angioedema in susceptible patients?
- Angiotensin-converting enzyme inhibitors
- Phosphodiesterase inhibitors
- Calcium channel blockers
- Beta blockers
- Alpha-adrenergic blockers
Which of the following blood pressure medications is most likely to cause hypokalemia?
- Thiazide diuretics
- Angiotensin-converting enzyme inhibitors
- Angiotensin II receptor blockers
- Calcium channel blockers
- Beta-blockers
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |