Playlist
Show Playlist
Hide Playlist
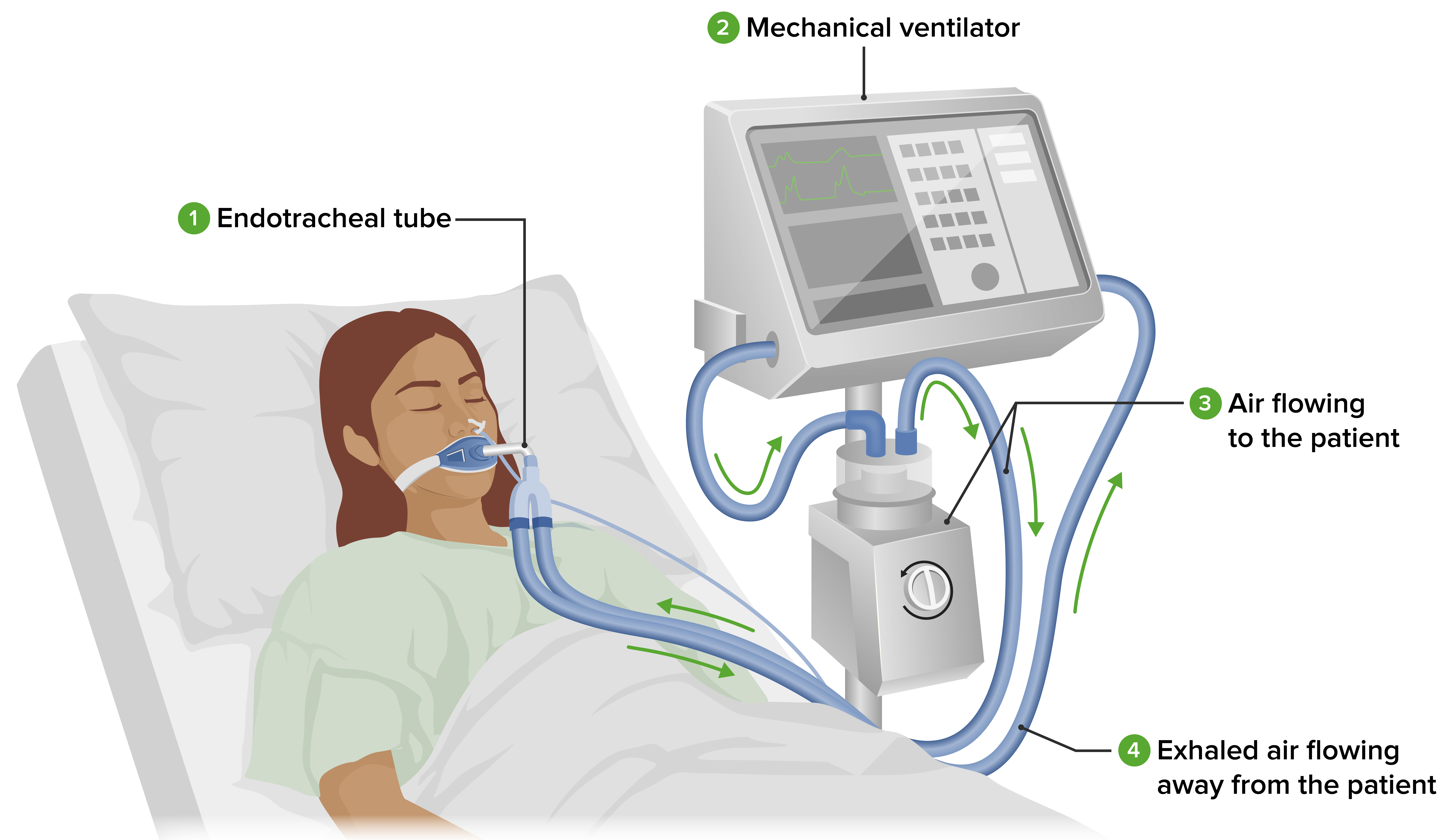
Mechanical Ventilation
-
Slides RespiratoryFailure RespiratoryPathology.pdf
-
Download Lecture Overview
00:01 Now, all that I wish to do here is introduce the terms here. And then in the next topic, we’ll go into definitely what the modes will look like with the graph and how to interpret your graphs based on the type of mode of ventilation that you wish to provide. We’ll have assisted control, we’ll have what’s called intermittent and then pressure control. 00:19 FiO2, what does that mean? Good. Are you picturing this? FiO2, the prime example that I’ve given you over and over again is high altitude. Why does FiO2 drop there? Because of barometric pressure. In a hospital setting, what might you wanna do with FiO2? Literally, the parameter that you can change. 00:39 Tidal volume and respiratory rate. I just went through a table to clearly highlight those two patients of rapid shallow breathing versus rapid deep breathing. You tell me, what’s more important to increase your alveolar ventilation, which is the objective? Very good. It’s your tidal volume, isn’t it? Because you want to make that dead space as negligible as possible. So, therefore, by increasing tidal volume and we’re going through rapid deep breathing there, as a compensation for DKA. But, understand though, clinically speaking, the respiratory rate and also increasing tidal volume will then give you a profound increase in your alveolar ventilation. Are you seeing it? If you don’t, go back to discussion, please, about our alveolar ventilation. 01:30 And then, we have positive end expiratory pressure. I’ll show you a graph here that will quickly show you what the difference is in terms of breathing with a positive pressure versus a normal, negative pressure. Let’s take a look. 01:44 Here, we have a graph explaining two patients that are receiving, well, PEEP specifically, but then patient B has PEEP + 8 cm of water that he or she is receiving. We’re gonna walk through this so that you clearly see the advantages of PEEP itself and then understand as to what some of these important disadvantages might be. 02:11 We have patient A in orange. The X-axis then represents the breathing rates or rhythms and the Y-axis then represents the pressure. Let us now begin at FRC. What does FRC mean to you? It’s ground 0. Here, for patient A, literally is 0. But theoretically, don’t try this at home, it’s your epiglottis being open with no air moving in or out. That’s the definition of FRC. So, this is a functional residual capacity. Zip. 02:41 Okay, so, now, you’re gonna begin breathing. Now, upon breathing, you’re gonna have inspiration that’s taking place that takes you to the increase in spike. And at the end of expiration then, obviously, alveoli becomes smaller. But this is dangerous. Say that you have a patient who requires oxygen is in a state of respiratory compromised and your patient is at risk for, guess what? Atelectasis. What might you want to do to make sure that alveoli, because, remember, if that alveoli shuts, that surfactant has a really hard time protecting the alveoli from maintaining or trying to keep open. So, therefore, the more, remember, and this is once again that the normal stuff that you wanna know. If it’s surfactant, it protects whom better? An open alveoli. It protects a smaller alveoli even a little bit better, doesn’t it? Because that’s what requires the decrease in surface tension. Surfactant, amazing name actually. And so, therefore, you wanna at least keep that alveoli alive and open, so that things do not collapse. Is the objective understood? Let us now take a look at patient B. 03:58 So, normally speaking, how was it that you open up your alveoli? Inspiration, pleural pressure becomes more negative. The more that the lung becomes negative, what happens to the alveoli? Ah, it expands. But now, you are going to become the lung. You, the clinician. 04:15 You’re going to become a mechanical lung. So, therefore, how do you keep that? How do you keep that alveoli open? You have to introduce positive pressure into the airways. 04:26 So, you introduce positive pressure, along with it, well, you have it at 8 cm of water. 04:31 That’s quite a bit of pressure, can you imagine? And with that positive pressure, you then maintain even at the end. So, I want you to come down where it says positive PEEP. 04:39 It stands for positive end expiratory pressure. So, at the end of expiration, there’s still positive pressure that is then maintaining the patency of the alveoli. And you noticed that here, even at the end, we’re still as high as +8. That’s a lot of positive pressure in your alveoli to keep it open. Is that clear? Completely the opposite of what? Negative, normal. 05:06 So, now, what are some of the major disadvantages that you’re worried about? Well, the major disadvantage of PEEP is the fact that you might introduce so much positive pressure, you might then cause compression of the pulmonary capillaries because they’re right there. 05:20 That membrane is so small of the alveoli, right across the street is whom? The pulmonary capillary. And so, therefore, think of it as being an avalanche. 05:30 Think of a tiny road and there is all those rocks falling. It completely obstructs the road and the road no longer, well, there’s no cars moving. In other words, there’s no blood moving, same thing. So, that alveoli is at this point introduced positive pressure, exerts the effect across the street or on the street which then represents the blood vessel and gone is the blood vessel, right? Wow, if the pulmonary capillaries are now, well, obstructed, who is going to fill the effects? Good. The right side. May result in right ventricular type of failure. is that clear? So, understand in the long run, what kind of effects that you wanna use or exercise caution with when utilising tools such as positive end expiratory pressure.
About the Lecture
The lecture Mechanical Ventilation by Carlo Raj, MD is from the course Respiratory Failures.
Included Quiz Questions
Which of the following statement regarding positive end-expiratory pressure (PEEP) is correct?
- PEEP treatment might be effective in patients with an acute decrease in functional residual capacity (FRC).
- It is a mode of therapy never used in conjunction with mechanical ventilation.
- At the end of exhalation, PEEP maintains the patient's airway pressure below the atmospheric level.
- PEEP works by exerting pressure that does not oppose passive emptying of the lung.
- PEEP treatment is very ineffective in patients with diffuse lung disease.
What happens to the alveoli with the use of positive end-expiratory pressure?
- Keeps the alveoli open even at the end of expiration
- Keeps the alveoli closed at the end of expiration
- Keeps the alveoli in a state of immobility
- Keeps the alveoli closed at the end of inspiration
- Keeps the bronchioles open at the end of expiration
Which of the following is a common complication of positive end-expiratory pressure ventilation?
- Obstruction to the flow in the pulmonary capillary
- Lung infection
- Hypercapnea
- Volutrauma
- Interstitial emphysema
Customer reviews
1,0 of 5 stars
| 5 Stars |
|
0 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
2 |
2 customer reviews without text
2 user review without text