Playlist
Show Playlist
Hide Playlist
Introduction to Male Reproductive Pathology
-
Slides Introduction Male Repro.pdf
-
Download Lecture Overview
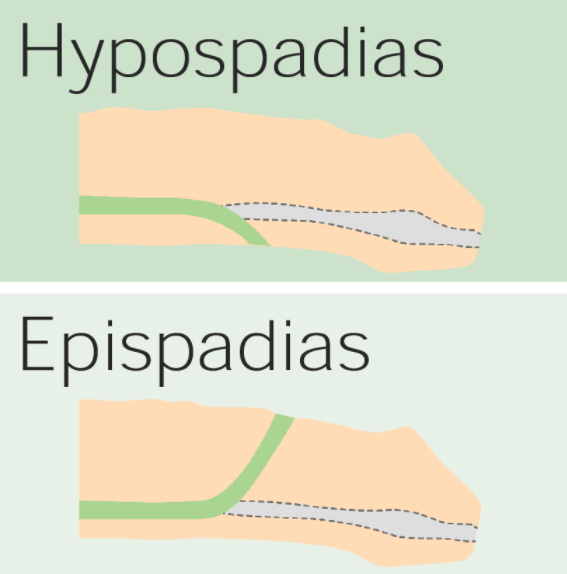
00:01 Here we’ll take a look at the male reproductive pathology. 00:03 And just like we have done in many organ systems, we shall also approach this in an organized fashion. 00:09 Let’s begin. 00:13 We’ll begin our discussion by looking at congenital male reproductive pathology and here, you’ll notice just a couple of topics in which which I’ve kind of integrated them so that you can get a good idea as to what you can expect in terms of development of the testis. 00:29 If you notice a picture on the left -- So this will be embryologically. 00:34 If you notice on the left that the fetus and the testis are located up in the abdomen. 00:40 And at some point in time, the gubernaculum, which you see in picture B here is going to literally pull the testis down into the scrotum. 00:49 And there’s a condition in which, if at any point in the testis do not properly descend into the scrotum, we have problems of undescended testis. 00:59 In other words, cryptorchidism. 01:01 We’ll talk about that in greater detail when we talk about testicular tumors. 01:05 Anytime there is cryptorchidism or there is improper descent of the testis into the scrotum, then you’re worried about cancer developing in your male, unfortunately. 01:17 Next, we have a little structure here called the processus vaginalis. 01:21 Just a quick little overview of anatomy here. 01:24 And on the bottom, you’ll notice numbers. 01:27 And number one, when we get to letter D here in the illustration, is what if you had openings either on the dorsum or the ventral aspect of the penis. 01:38 You call this either hypo- which means the bottom, but more importantly, make sure that you know the description of it. 01:45 So even though this is bottom of the penis, you then call this what? The? Good. 01:50 Ventral portion. 01:51 Clear? So now, what is your patient what is your child predisposed to? Infection. 01:57 Infection. 01:58 Hypospadia more common than epispadia but there are complications that you want to know for both. 02:04 In hypospadia, it is once again the ventral portion of the penis that is failure to fuse if you remember from embryology. 02:12 Whereas epispadia, as the name implies, would be the – Well, that would be the top of the penis, but they’re not going to say “top of the penis.” Clinically, they’ll call it what? The dorsum. 02:20 Same concept. 02:22 What’s the dorsum of your foot? When you say dorsiflex, what are you doing? You’re taking the foot and you’re moving it towards your leg, aren’t you? Well, here, you have the top of the penis, which is the epispadia. 02:31 Failure to fusion here, what’s your complication in a child? It’s called bladder extrophy. 02:37 E – epispadia. E – extrophy. 02:41 Now the complications as I said, hypoaspadia is more common than epispadia. 02:45 Take a look at number one so that you know as to where you are vicinity-wise. 02:49 Number two, as the name implies, well, bladder exstrophy. 02:52 But in addition to that, there are a couple of other things here that you want to know. 02:56 If you have failure of your lateral fusion of your abdomen, then you can have what’s known as an omphalocele. 03:03 And an omphalocele would mean that you have herniation of the abdominal organs in a child. 03:09 And when this happens, it is still covered by the peritoneum. 03:12 Keep that in mind. 03:13 Omphalocele, the failure of lateral fusion. 03:16 In embryology, we’ve also looked at gastroschisis and that would mean that the peritneum is not covered. 03:22 A couple embryologic issues. 03:24 Hydrocele: Well, with hydrocele (see number 3), what ends up happening is that there’s accumulation of fluid surrounding the testis, between the visceral and parietal layers of the tunica vaginalis. 03:38 And we’ll talk more about hydrocele when the time is right and we’ll compare hydrocele to varicocele. 03:43 And for us, varicocele will play more of a role in pathology, but hydrocele, just as important. 03:50 A quick little overview of your embryology and then some of the associated pathologies that you’ve seen. 03:55 Let us keep moving.
About the Lecture
The lecture Introduction to Male Reproductive Pathology by Carlo Raj, MD is from the course Male Reproductive System Diseases.
Included Quiz Questions
Which condition is associated with hypospadias?
- Urinary tract infections
- Penile squamous cell cancer
- Painful sexual intercourse
- Red discoloration of the skin
- Testicular cancer
Which physical finding leads to omphalocele?
- Failure of fusion of lateral abdominal folds
- Failure of fusion of cranial abdominal folds
- Overmigration of lateral abdominal folds
- Failure of fusion of caudal abdominal folds
- Overmigration of medial abdominal folds
What is the MOST accurate definition of epispadias?
- Opening of the urethra located on the dorsum of the penis
- Opening of the urethra located on the ventral aspect of the penis
- Opening of the urethra located on the lateral surface of the penis
- Opening of the urethra located on the scrotal wall
- Opening of the urethra located on the base of the penis
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |