Playlist
Show Playlist
Hide Playlist
3 Types of Cartilages
-
Slides 07 Types of Tissues Meyer.pdf
-
Download Lecture Overview
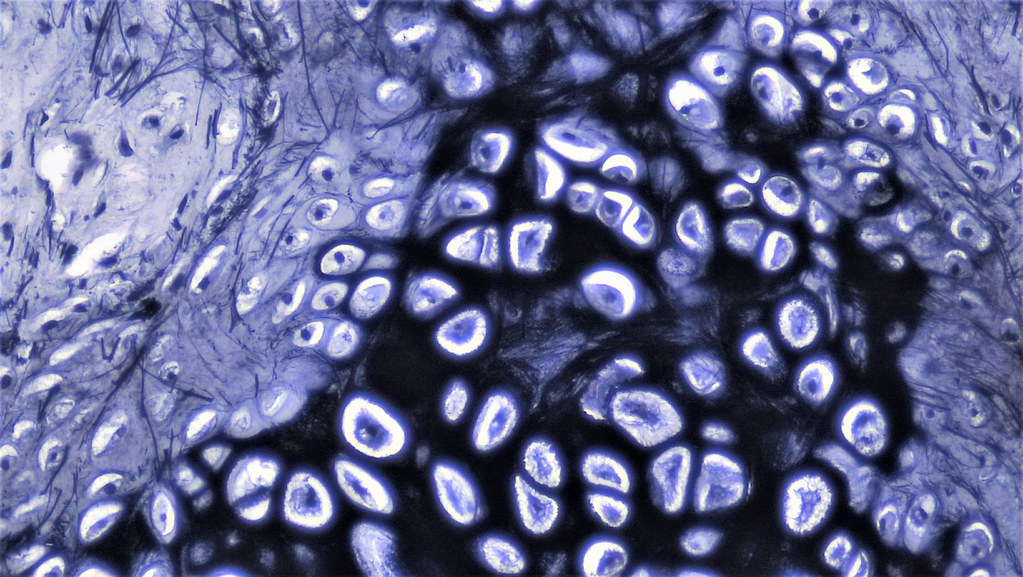
00:00 As I mentioned in the very start of this lecture, there are three types of cartilage. So let us have a look at these three types of cartilages. 00:10 It is very important that you know how to distinguish each of these three types of cartilage and also it is important for you to understand the functional role each of these cartilage has in various locations of the body. Remember though, that even though there are three types of cartilage, each of these cartilages contain cell,s chondrocytes. They each contain the glycoaminoglycans that are so important in maintaining a lot of water content and resisting compressive forces. They also contain proteoglycans and also glycoproteins that are also very important in stabilising the extracellular matrix and making sure the cells adhere to most components of the extracellular matrix. By far the most common type of cartilage is hyaline cartilage. 01:14 We will have a look at that in more detail, but it contains basically collagen type II. 01:21 We have elastic cartilage in certain locations of the body and as the name suggests, they contains predominantly elastic fibres, although there is collagen in this type of cartilage as well, giving it some sort of support. And the last type of cartilage is fibrocartilage. 01:40 As the name suggests, it is very very fibrous. It has a network of strong collagen type I fibres. It is very much like dense regular connective tissue such as a tendon or a ligament. And it is often difficult to distinguish fibrocartilage from dense connective tissue that is regular. So let us look at hyaline cartilage first. As I said earlier, it is the most abundant form of cartilage in the body. Have a look at this image that you have seen before. See if you can point out to yourself, a chondrocyte. There are many here in this image. Sometimes you can see the chondrocytes appearing in pairs and those pairs we call isogenous groups. Sometimes they are in collections of three or four. And I will mention again these isogenous groups later on, when I talk to you about the growth of cartilage. 02:50 When you look at this image and you see the matrix, you can see that it is different colour in different locations. If you look very closely around the chondrocyte, you can see that the matrix has a very bluish tinge and we call that the capsular or the pericellular matrix. 03:12 That matrix, very close to the cell. Further out, we have territorial matrix around the cell, which looks very bright pinky reddish colour and then finally we have matrix further out, away from the chondrocytes called the interterritorial matrix. I do not think it is really important to worry too much about understanding the names of all these areas of the matrix. The reason why I mention it here is because it just reflects the concentrations of matrix components as they are secreted by the cell. They are secreted by the chondrocytes and therefore they stain a lot more dense. Then when they begin to diffuse out and rearrange themselves further out in the matrix separated away from the cells. So it really reflects the different compositions of the matrix as the cell is producing that matrix and forming the matrix. So these staining differences, although they are not important for you to memorize and they are not really an important part of the histology of cartilage, they just merely reflect the very active chondrocytes, particularly during developing cartilage. 04:37 These chondrocytes were busy every day making sure that the matrix components are replaced because some of them have rather short half lifes, some have very long half lifes. So they are busy busy cells. Well, let us continue looking at the matrix of hyaline cartilage. It is clear or glassy, hence the name hyaline. But also understand that there are many different collagens that are embedded in the extracellular matrix of this cartilage. When I described collagen, the structure of collagen in a general connective tissue lecture, I explained that the collagen fibres are made up of collagen fibrils, each made up of individual collagen molecules. And the collagen molecule itself consists of three alpha chains of polypeptides. These polypeptides can contain between 600 and 3000 different amino acids. So because of that, there are different collagens in the body. In general connective tissues, I mentioned only collagen type I and collagen type II and collagen type III because they are the main collagens that we will come across in this histology course. But in this particular image you see, there are a list of different collagens that as I said earlier, are embedded in the extracellular matrix. And what these collagens do is they bind the extracellular matrix together. 06:34 They combine or they bind the matrix with the cells, with other proteins, with other glycoproteins and they create a three-dimensional lattice in the extracellular matrix. And that is very important for the chondrocytes because they detect compressive forces. They detect the stresses that are imparted on the extracellular matrix. They have the ability to sense all sorts of mechanical stresses. It is like you going and lying on a mattress, a soft mattress or a hard mattress. You can tell the difference. Similarly, the chondrocytes also can tell the difference and they continually adjusting the matrix components to make sure that the matrix is of the right components, the right constituents, to be able to fulfill the role to which it needs to be designed, resisting compressive forces also being flexible and so on. 07:46 Hyaline cartilage is found at the surfaces of joints. Their job here is to be cushions and to resist compressive forces. They are friction free surfaces at joints. They are lubricated by synovial fluid. In this section, you can see two opposing bones joined together but separated by a very thin space, which is filled with synovial fluid and the surface of the bone has articular cartilage upon it. Now that synovial space is filled with synovial fluid secreted by a synovial membrane on the outside of the joint. It is very difficult to see here and the joint is supported on the outside by ligaments. But this articular cartilage is designed, as I said earlier, at a joint to resist compressive forces and to act as a cushion and a friction free surface for joint movement. If you look at very high magnification of the articular surface of cartilage, then it has really four different zones. Have a look at the arrangement of the chondrocytes at the very peripheral part of the cartilage, at the edge of the joint or in contact with the synovial fluid. That synovial fluid not only lubricates the joints, but it provides nourishment for the cartilage cells. 09:31 Remember I said that cartilage is avascular. Well, the way in which cartilage gets its nutrition is because the extracellular matrix has a watery soluble component, an aqueous component. So nutrients can very readily move through those aqueous components of the extracellular matrix and, therefore, the chondrocytes can get their nutrition. In the case of articular cartilage, the nutrition comes to these cells through the synovial fluid. But there are different zones you see in the articular cartilage. There's a superficial zone with a cartilage cell seem to be elongated parallel to surface. The intermediate zone where they tend to be lining rather randomly throughout the articular cartilage and there's a deep zone where they tend to be lined up in columns. And there is a further area, right outside, next to the bone where the cartilage tends to be calcified. Now those four zones although it is often difficult to distinguish between each of those zones just looking at the cartilage, it is easy to distinguish the zones if you could have a look at through arrangement of the collagen. We cannot see that there, but in special preparations, you will find that in the superficial zone, the cartilage is arranged parallel to the surface. In the intermediate zone, the cartilage is arranged in a more random criss cross networking type arrangement. 11:13 And towards the deeper zone, the collagen fibres are arranged along the long axis of the bone and this arrangement is ideal for articular cartilage to be able to withstand compressive forces coming down onto the joint during movement and because of body weight and gravity. Now you cannot see in this slide, but just adjacent to the calcified zone of cartilage, towards the synovial joint is an area where the cartilage cells are constantly dividing and replacing other cartilage cells that have limited lifespan at the very surface component of the joint. Another place in which we find hyaline cartilage is supporting certain structures. Here you see an image through the trachea and also the external ear canal. 12:15 These are areas where you really need a very strong support. You can feel the cartilage rings in your throat yourself. If you did not have cartilage there, your trachea or your major windpipe going down to your lungs would collapse. So cartilage here is very important to maintain an open airway and we will look at this type of cartilage again when we look at the respiratory system later on, similarly with the external ear canal. 12:51 One of the remaining functions of hyaline cartilage is it acts as a fetal skeleton. And during development of bone, that fetal skeleton of cartilage, that template of cartilage is replaced by bone. Now be very careful to hear what I said a moment ago. I said that the cartilage is replaced by bone. The cartilage does not turn into bone and that is an important issue that we need to remember when I will talk to you about the growth of bone and the formation of bone in a later lecture. Elastic cartilage quite obviously has got predominantly elastic fibres within it. In a normal H&E section stain here, you can see the elastic fibres. Remember from connective tissue lectures in a general description of the elastic tissue, elastic fibres are branched fibres. And although you cannot see in detail here, they also interact with the collagen fibres in this type of cartilage, but the prominent component of elastic cartilage as the name suggests is elastic fibres. 14:18 And that is important to maintain flexibility support, strong support, but also flexibility of the structures where you find elastic cartilage. And one place you find it, is in the pinna of the ear shown here. I can twist my ear around and then let it go and it springs back to place because of the flexible elastic cartilage within it. Well, the other remaining type of cartilage is fibrocartilage. As I said earlier, it is very similar to dense connective tissue. It is often difficult to tell the difference between fibrocartilage and dense connective tissues. Here you see it in a joint in the vertebral column. 15:15 It is important to be in the joint of the vertebral column where we need to withstand very strong compressive forces, particularly during movement, but also body weight forces that are passed down the vertebral column. And again if you look at the section, you can see lots and lots of pink stained collagen predominantly collagen type I is there, which is a very strong thick collagen, but there's also type II collagen there that you find in hyaline cartilage. And sometimes in the intervertebral joints that you see on the right-hand side, if you could look at that joint under a microscope, you would see hyaline cartilage there as well as fibrocartilage. 16:05 And that is often difficult to see the two, unless you look for these very strong deep stained bands of collagen type I within the fibrocartilage. Again look at the chondrocytes, you can see little tiny dots of chondrocytes. The very clear space around the chondrocytes that you would have noticed looking at hyaline cartilage earlier is called a lacuna. 16:31 Normally the chondrocyte would occupy the entire space. Think back on that slide or image of hyaline cartilage, where all you saw of the chondrocyte was a little tiny dark dot representing perhaps the nucleus or the debris of the cell after all the processing has taken place for you to review it under a microscope. But normally the lacuna space is really occupied by the entire cell. It is just an artifact really due to shrinkage of the cell during processing. 17:11 The sorts of places where you find fibrocartilage is obviously where you want to withstand very strong compressive forces such as the intervertebral disc, the symphysis pubis in the pelvic joint, the temporomandibular joint to withstand the compressive forces of chewing, and also the menisci of the knee to again withstand the forces or the compressive forces particularly during movement and the dissipation of body weight down through the body.
About the Lecture
The lecture 3 Types of Cartilages by Geoffrey Meyer, PhD is from the course Connective Tissue.
Included Quiz Questions
Type 2 collagen is the basis for which of the following?
- Hyaline cartilage
- Keloid
- Newborn skin
- Scar tissue
- Dermatofibroma
How many types of cartilage are there in the human body?
- 3
- 4
- 2
- 6
- 5
A collagen molecule is composed of which of the following strands?
- Polypeptide
- Glycoprotein
- Myosin
- Carbohydrate
- Lipid
Which of the following types of cartilage may be found as a translucent cartilage over joint surfaces?
- Hyaline cartilage
- Articular surfaces of bones do not contain cartilage.
- Elastic cartilage
- Fibrocartilage
Elastic cartilage is primarily found in which of the following?
- Pinna of ear
- Tracheal rings
- Intervertebral disk
- Articular surfaces of bone
- The pubic symphysis
Which of the following structures is primarily fibrocartilage?
- Annulus fibrosus of the intervertebral disk
- Tracheal rings
- The cricoid
- Ribs
- Pinna of ear
Customer reviews
4,0 of 5 stars
| 5 Stars |
|
3 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
1 |
All of the lectures by prof. Meyer are absolute blast and great experience.
Hola! No han solucionado el problema y se los avisaron hace 4 meses. 4 months ago Soe S. said you that the transcription has a problem of 1 minute of length.
Everything was clearly explained, especially helpful in the times of the pandemic. Thank you very much professor!
Solid review and helpful information in regards to histology. The slides are helpful