Playlist
Show Playlist
Hide Playlist
Tracheoesophageal Fistula and Esophageal Atresia
-
Slides GIP Tracheoesophageal Fistula Esophageal Atresia.pdf
-
Download Lecture Overview
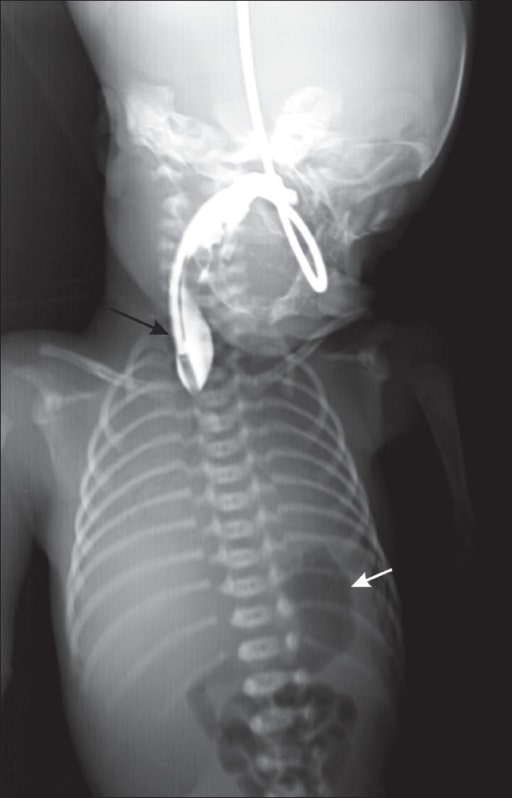
00:01 Welcome. In this talk, we're going to cover tracheoesophageal fistula and esophageal atresia. 00:07 And it may seem like we're talking about two very different things. 00:10 In fact, as you'll see developmentally, they kind of go together. 00:14 So esophageal atresia formally is just where we've lost a segment of the esophagus. 00:21 It doesn't completely develop. So we end up with a functional gap. 00:25 They may even be the two ends of the esophagus may be connected by a fiber strand but nothing can get through it. 00:33 That's esophageal atresia. 00:35 On the other hand, a tracheoesophageal fistula is an abnormal connection between the esophagus and the trachea. 00:42 So we're seeing here atresia because the esophagus is interrupted but we're also seeing a fistulous tract where the lower segment of the esophagus actually connects to the trachea. 00:55 This association is actually the most common of the various fistulas and/or atresias that can occur involving the esophagus and the trachea. 01:07 And then, finally, we have this entity which is a fistula without atresia. 01:11 So a connection between esophagus and trachea but the esophagus itself is one continuous tube and everything flows down that way. 01:20 With this though, you can probably anticipate that there are going to be problems because of the abnormal connections and/or the gaps that can occur within the esophagus. 01:30 So let's talk about how those play out. First, we'll do a little bit on the epidemiology. 01:36 So this is showing the most common of the various anomalies involving the esophagus and the trachea. 01:42 It's a combination of atresia. 01:44 So that gap between the top and the bottom of the esophagus and an associated tracheoesophageal fistula. 01:51 Altogether, this particular combination occurs about 85% of the cases involving the esophagus and the trachea and those anomalies. 02:01 When this happens, there is going to be a number of development abnormalities that are secondary to the fact that the GI tract is no longer a continuous tube from top to bottom. 02:13 In the absence of that continuous tube in the ability of the fetus to swallow amniotic fluid and move it through the GI tract, in fact, there will be too much amniotic fluid, so called polyhydramnios. 02:25 There are a number of associated findings that come along with tracheoesophageal fistula and/or esophageal atresia. 02:34 The acronym for this is VACTERL, V-A-C-T-E-R-L. 02:39 Not a great acronym because it doesn't really mean anything but it does succinctly describe a lot of the associated abnormalities. 02:47 So let's look at those in turn. The V stands for vertebral defects. 02:53 And in fact, the number of the defects under VACTERL are occurring because of some underlying genetic disorder. 03:02 So a syndrome and the esophageal atresia or the tracheoesophageal fistula's just part of that. 03:08 Some of the defects that we're going to talk about in VACTERL are actually coming from the fact that the baby is not able to swallow amniotic fluid. 03:17 But the vertebral defect by and large is part of a syndromic genetic something going wrong overall with the development of the baby. 03:26 A stands for anal atresia. 03:28 This may be primary or it may be related to the fact that the baby's not able to swallow and passage the fluid from the amniotic sac. 03:39 C are cardiac defects. These are probably part of the underlying genetic basis of the disorder. 03:46 T and E for VACTERL, the T and E are the tracheoesophageal fistula and/or esophageal atresia. 03:58 R stands for renal anomalies. 04:01 And again, this may be part of the underlying genetic disorder or it may be because the baby's not passaging fluid in a normal way. 04:09 So the fluid is not going across just down the GI tract, but in fact, is being absorbed and may be part of the normal, renal development. 04:18 And finally, limb abnormalities. 04:20 And again, the limb abnormalities may be part of the basic genetic syndrome or it could be because of all the abnormal amount of amniotic fluid that's left behind and there may not be typical development of arms and legs. 04:34 So the pathophysiology, the normal tube that's going to become the bronchial tree and the esophagus is one central midline tube early on. 04:45 There's a ventral aspect that will become the bronchial tree and there is a dorsal aspect that will become the esophagus. 04:52 During normal development, the ventral aspect will branch and then, branch and branch again to produce the bronchial tree. 05:02 The posterior aspect will separate out and become an esophagus whom we will form a separation between that with a combination of smooth muscle and epithelium. 05:14 In the setting where we don't have complete development of that dorsal aspect, the tube that's going to become the esophagus, we have esophageal atresia. 05:23 So we have a segment that has become stenotic or frankly, completely absent. 05:29 On the other hand, when we form a tracheal esophageal fistula, we have our ventral area that's going to be the bronchial tree. 05:38 We have the posterior or dorsal aspect that's going to become the esophagus. 05:43 And then, during development, we end up with either a complete gap, so we have atresia of the esophagus and we also have an area where the esophagus is connected aberrantly to the bronchial tree, so a tracheoesophageal fistula. And what we're seeing here is the one that - one entity, the one malformation that is the most common of all the different forms of esophageal atresia and/or tracheoesophageal fistula. 06:13 The exact etiology remains unknown. There's very likely a genetic component because half of the cases have all those associated malformations, remember VACTERL. 06:24 The clinical presentation based on what you've already seen kind of comes from first principles. 06:30 There may either be an abnormal connection between the esophagus, so when the baby swallows, it goes into the bronchial tree. 06:40 Not good. On the other hand, you may have air going in to the rest of the GI tract as the baby inhales and we have air going through a tracheoesophageal fistula down into the lower end of the esophagus, the stomach, and duodenum. 06:58 So in the infant who has one of these anomalies, the symptoms usually manifest pretty early, usually, within the first 24 hours. 07:08 With esophageal atresia where there is not a complete formation of the esophagus and there's gap, the baby will have drooling, an inability to feed, and regurgitation. 07:19 Now, this is completely an absence of anything connecting the esophagus to the trachea. 07:24 This is just atresia. In tracheoesophageal fistula however, every time the baby ingests something or even just salivates, that is going to be going into the lungs, not a good situation, because now, the baby's going to have respiratory distress. 07:41 The baby's going to have coughing and choking. 07:44 Baby will likely develop an aspiration pneumonia and the baby, because there is now probably a distal connection from the trachea into the lower GI tract, every time the baby inhales, there will be now air going into the stomach, so there will be abdominal distention, basically, hyper-inflating the GI tract. 08:07 So the diagnosis, not a hard one based on what you're seeing there, but nevertheless, one that has to be recognized very early on, otherwise, the baby will get into a lot of trouble. 08:18 So on physical exam, a simple thing is that frequently, if there's drooling and the baby's not apparently able to move fluid from top to bottom, we'll pass a nasogastric tube or will attempt to do that. 08:32 In a setting of esophageal atresia, you put it in there and it doesn't go anywhere. 08:37 So it will often come back out as you do that. 08:40 If there is a tracheoesophageal fistula such as you see here with the dotted line and the arrow, there will be abdominal distention. 08:48 Baby - every time the baby inhales, air is getting out into the GI tract and it'll just inflate the stomach. How can we see this on imaging? So a plain radiograph frequently will help you make the diagnosis. 09:03 You may see a completely gas filled gastrointestinal tract that says you probably have a tracheoesophageal fistula. 09:10 On the other hand, the nasogastric tube, you can see it here is that very electron-dense line that's coming from the head area down, trying to go into the esophagus, curls up, and comes back up. 09:25 So that's saying that we have esophageal atresia. 09:27 You may also, if you have just isolated esophageal atresia, so no fistula, just atresia, you may have an entirely gasless abdomen. 09:38 And usually, the baby is sucking down some air. 09:41 So there should be some air, just shouldn't be hyper-inflated. 09:44 What do we do about this? Okay. We need to recognize it quickly. 09:49 When we do recognize that this is going on, we want to keep the baby in the head up position. 09:54 We don't want to regurgitate gastric contents through a tracheoesophageal fistula into the lungs that will cause very nasty chemical pneumonitis. 10:03 We definitely want to provide nutrition, so we'll put them on total parenteral nutrition. 10:08 We are going to give them broad spectrum antibiotics just to protect against the possibility that they have aspirated. 10:14 And we're going to completely suction everything that ever falls into the esophagus just to keep that from regurgitating. 10:20 And then, we call our friendly surgeons and we say, "Dudes, you need to come in and you need to now reestablish normal flow across the atretic portion of the esophagus if present and you need to cut the connection between the esophagus and the trachea." The prognosis if we do everything that we're supposed to do and we recognize the entity early on, survival is quite good with surgical treatment and in fact, the early [inaudible 11:11] are usually not associated with the esophageal or tracheal anomalies but rather due to the other associated anomalies, the heart defects, the renal defects, etc. 10:59 And with that, we finish tracheoesophageal fistula and esophageal atresia.
About the Lecture
The lecture Tracheoesophageal Fistula and Esophageal Atresia by Richard Mitchell, MD, PhD is from the course Disorders of the Esophagus.
Included Quiz Questions
What percentage of tracheoesophageal abnormalities lead to proximal esophageal atresia with a distal tracheoesophageal fistula?
- 85%
- 75%
- 95%
- 99%
- 50%
What clinical finding is associated with a tracheoesophageal fistula?
- Vertebral defect
- Oligohydramnios
- Hepatomegaly
- Splenomegaly
- Diverticulosis
Which clinical finding is NOT associated with tracheoesophageal fistula?
- Splenomegaly
- Anal atresia
- Vertebral defect
- Limb anomaly
- Renal defect
What is an early symptom of esophageal atresia?
- Inability to feed
- Coughing
- Aspiration pneumonia
- Rapid weight gain
- Abdominal distension
What is a radiographic finding of esophageal atresia?
- Nasogastric tube curled up in the chest
- Right lung hyperinflation
- Air bronchograms
- Double bubble sign
- Tree-in-bud opacities
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
I liked the illustrations and the animations. the lecture was on point and easy to understand