Great review
By Alaena A. on 28. September 2022 for Hyperkalemia: Etiology & ECG
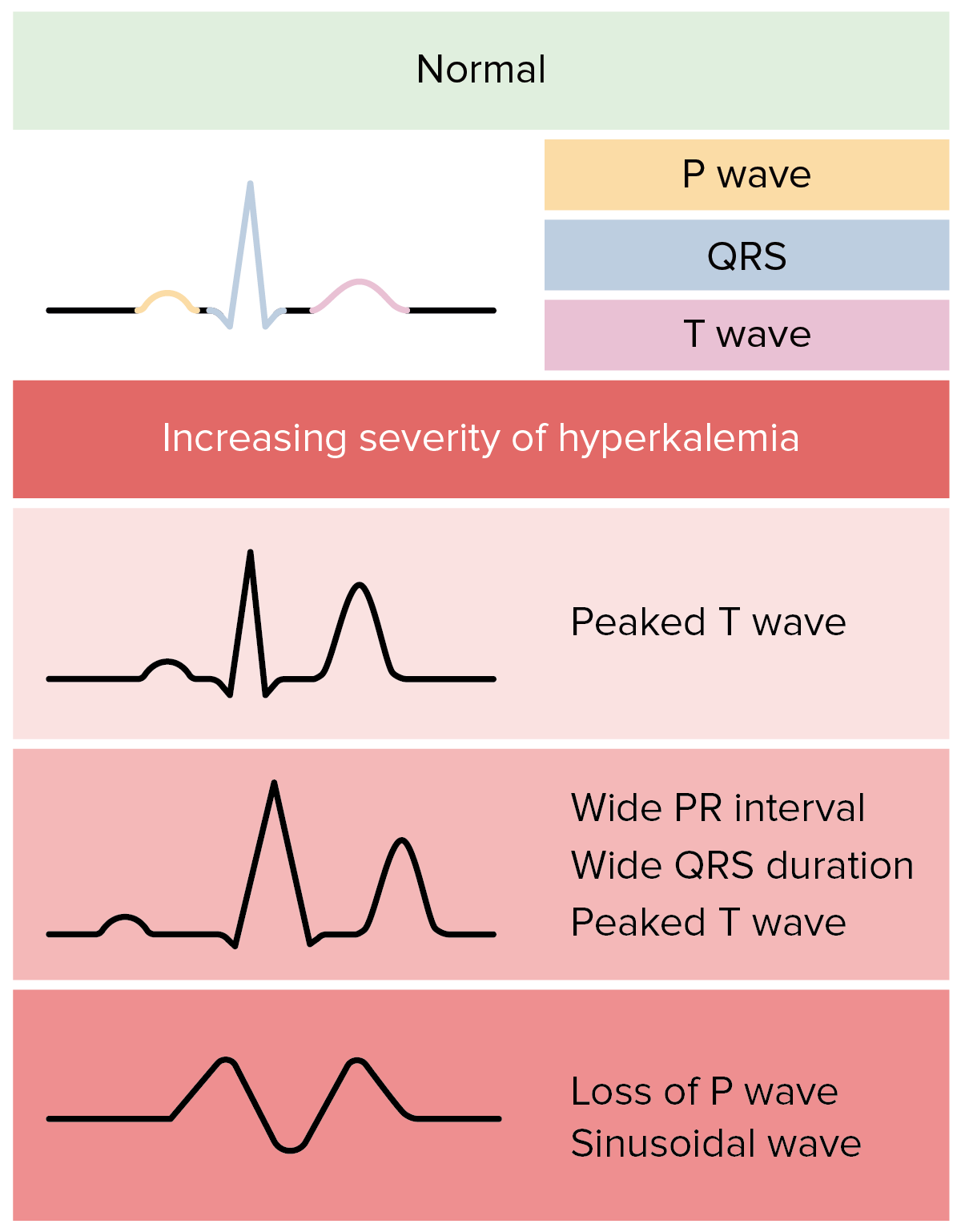
I really like Dr. Bord's explanation and back to basics review added here and there. I really like her explanation of the progression of changes you would see on an ekg.
Excellent!
By Ameli A. on 09. August 2022 for Endocrine and Electrolyte Emergencies
And efficiently synthetized course, keeping the most important points for reference.
Short, concise and very well explained. Love the slides too, thank you!
Excellent
By Dr-Nadeem N. on 26. April 2022 for Endocrine and Electrolyte Emergencies
Way of teaching is excellent with core clear concepts i really appreciate efforts of madam really suggest good stuff like that i hope more videos of madam soon.
Hypokalimia
By Ahmad A. on 03. July 2021 for Endocrine and Electrolyte Emergencies
the effects of renin angiotensin system
Hypo and hyperkalemia
Hypocalcemia and parathyroid hormon
Detailed Information
By Dengu D. on 10. June 2021 for Endocrine and Electrolyte Emergencies
Really a wonderful lecture! Thanks to Prof. Sarah Bord for the clear medical knowledge!
Quintessential lecture
By Noxolo Jessica Dorcas M. on 01. November 2020 for Endocrine and Electrolyte Emergencies
It was a quintessential lecture ,well detailed and the lecturer presents it well.
Great teacher
By Sha Ron u. on 28. August 2020 for Hyperkalemia: Etiology & ECG
Clear, succinct, and practical. Thanks for the lecture Dr Bord!
I like your lectures
By Zahra Muhammad S. on 21. June 2020 for Endocrine and Electrolyte Emergencies
The lecture series are awesome and explanatory. But please can you improve a little on the approach, by giving more details and on the topics being discussed.
Good teacher
By Theeranon T. on 08. April 2020 for Hyperkalemia: Etiology & ECG
It’s very useful information. Thank you. I’ll use the knowledge from this video for applying with my real work and it is beneficial for my patients.
Short lecture with exact points
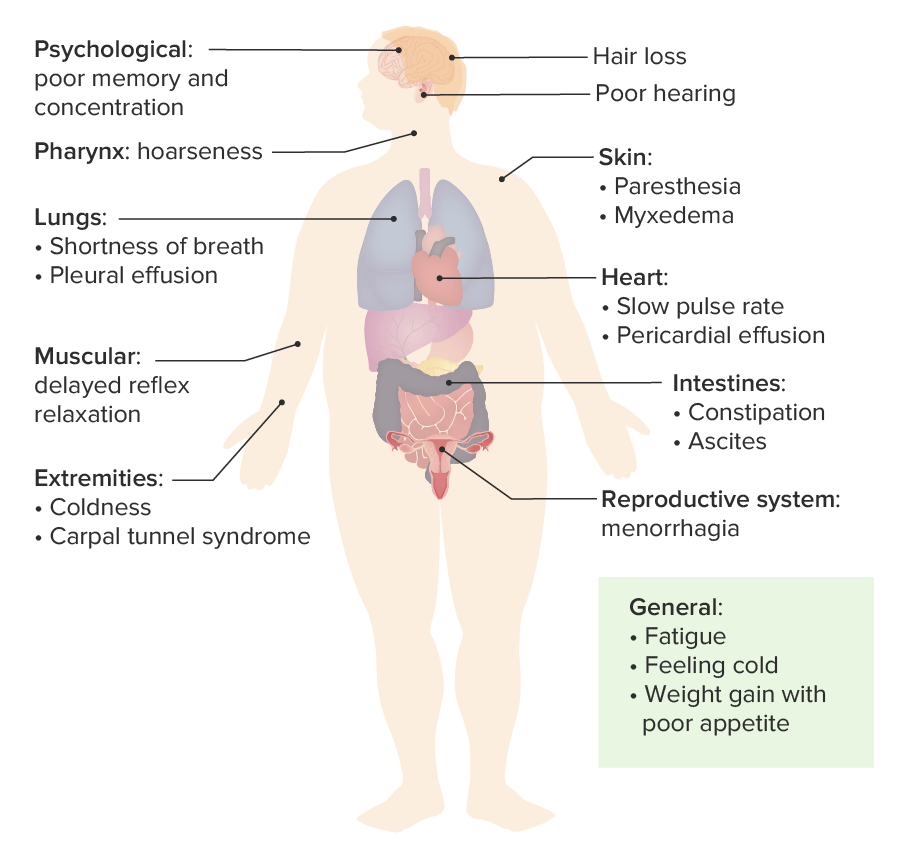
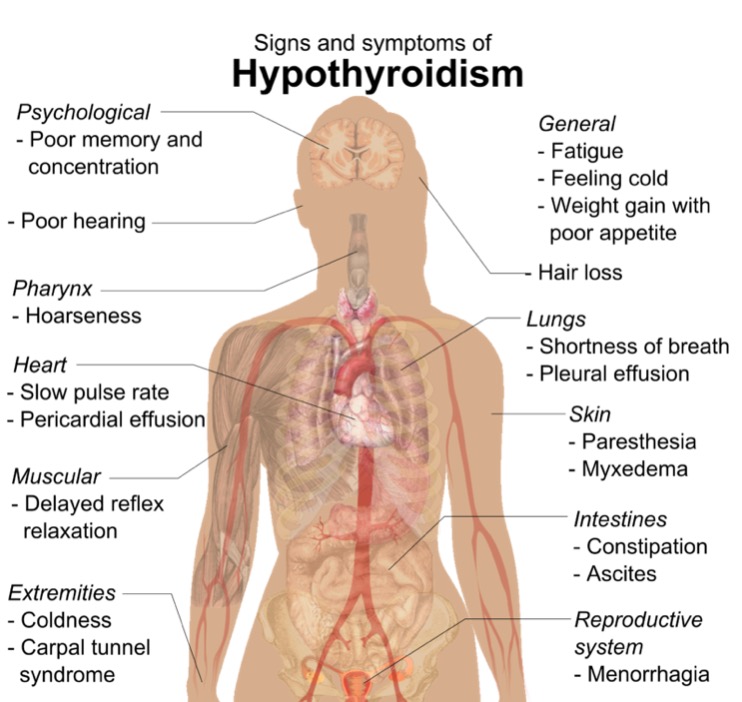
By Elvia A S. on 28. September 2019 for Hypothyroidism: Symptoms, Diagnosis, Treatment
Simple, concise lecture regarding hypothyroidism. Discussed - patient population, S/S, diagnostics, and treatments.
great
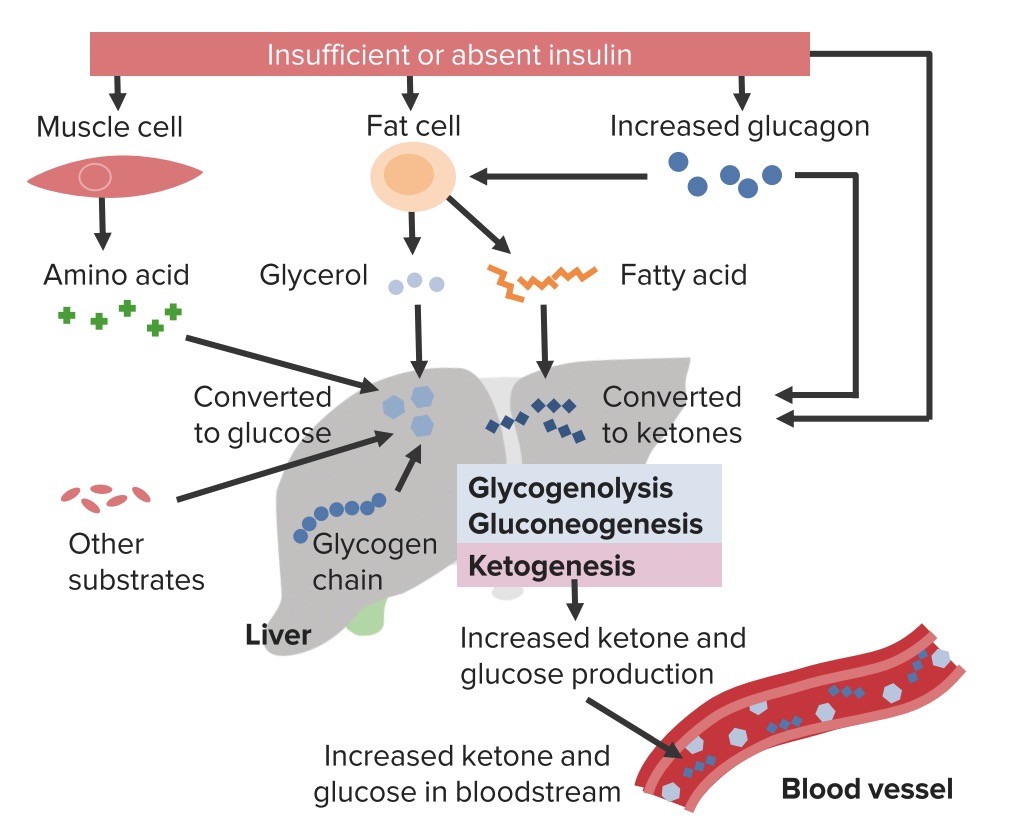
By Pia Trixy L. on 25. August 2018 for Diabetic Ketoacidosis: Pathophysiology, Physical Exam & Diagnosis
clear explanation and very good presentations. I love how she explains the causes and the pathophysiology
Thumbs up
By Michelle B. on 25. March 2018 for Endocrine and Electrolyte Emergencies
Dr Bord review was clearly presented. It makes it easy to remember
Short, concrete, useful review.
By Diana P. on 09. January 2018 for Diabetic Ketoacidosis: Pathophysiology, Physical Exam & Diagnosis
The reason I rate this as 5 stars is because it was a simple, concrete, and very useful way to remember the key points on DKA at the emergency department that is often full of patients. I'm writing from Colombia.
Good basic introduction
By tim h. on 24. November 2017 for Endocrine and Electrolyte Emergencies
Well designed and delivered, but content seemed more directed to pre-med audience.