Playlist
Show Playlist
Hide Playlist
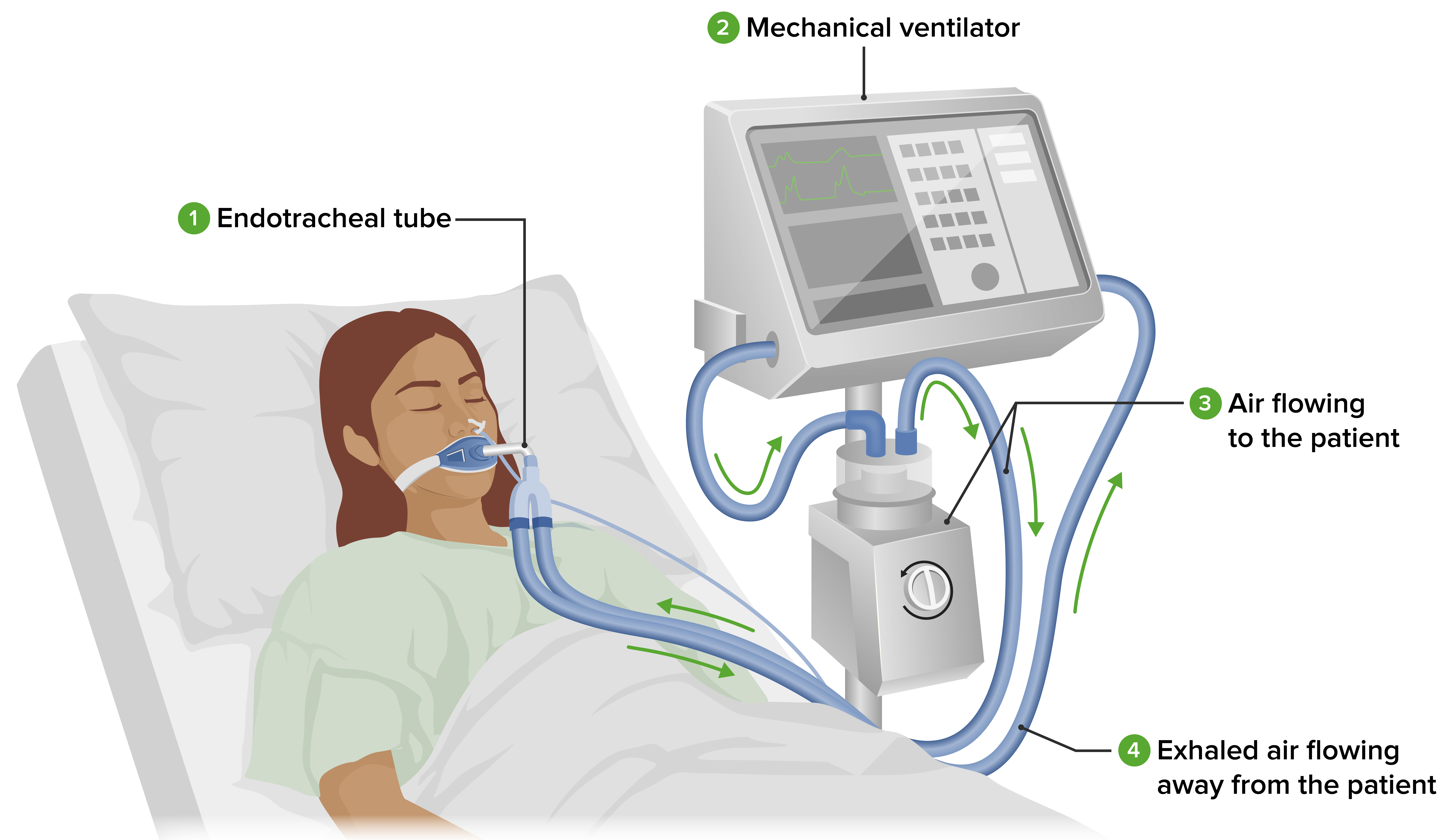
Modes of Ventilation: Mechanical Ventilation Goals
-
Slides ModesOfVentilation RespiratoryPathology.pdf
-
Download Lecture Overview
00:00 Continue. Okay, so goal of mechanical ventilation. Mechanical ventilation. So this obviously is invasive. Is that clear? So, if you talk about non-invasive, the test that you will be using for non-invasive. Remember, the one that we used for obstructive and restrictive? That was pulmonary function test. Was that invasive or non-invasive? You put a mask on the face. It might be invading your face, but you're not invading your mouth. Is that clear? So, you just put on a mask, that is non-invasive. You must understand that. 00:34 And now pulmonary function test was made up of what? FEV1 over FEC and that then puts you into the family of obstructive or restrictive, not to worry, we will go into those details about the pathology soon enough. 00:46 Now, at this point, however, your patient has and requires mechanical ventilation. 00:52 So this is definitely invasive. So these ventilatory graphs, that we're looking at here, become very important too. Minimize oxygen to avoid possible oxygen toxicity. What does that mean? Remember please, to drink a glass of water is fantastic, in fact, it is highly recommended. But, to drink out of a fire hydrant, it will kill you. Same concept. And oxygen, sure, vital, but if you give too much oxygen, what is that called? Reactive oxygen species or oxygen intermediates. You want to be careful for your radical damage. What else is the goal? Minimized PEEP. What does PEEP mean? Once again, positive end expiratory pressure. We had a full discussion of this earlier. Meaning to say that if you have too much PEEP, too much positive, why do I keep saying that? Because here, you are the lung, you are introducing positive pressure. I want to keep reiterating that because I want you to compare this to normal physiology in which if you want to inhale then you want that pleural pressure, or the individual, you and I right now, we are creating a negative pleural pressure. How many times have I mentioned this? Continue. But, if you have too much PEEP that means that you could then increase the volume within the alveoli so much that you might actually cause airway trauma and quite a bit of discomfort. So therefore mechanical ventilation is to then relieve some of that. 02:15 What is your goal? Obviously here, you want to increase your PO2. Your patient was already in respiratory failure type 1 or type 2. By definition, it means less than 60 and balanced effect of high FiO2. I will walk you through this. What is that FiO2 mean to you? Remember, normally speaking, it’s approximately 20%, isn’t it? And as long as you are at sea level, then you are going to multiple that 0.2 times 760. This is a patient that requires oxygen. What are you going to do in a hospital setting? You are going to increase FiO2, may be 0, 40%, maybe even 100%. But that is a lot of oxygen. So you balance the effects of high FiO2, understand every single physiologic point here. With the high effect of high PEEP, you want to balance these two ,because if you do not, then please understand, that you are going to be causing more harm than good. In some cases, you need both. For example, acute respiratory distress syndrome. 03:17 So, continue. These are goals of mechanical ventilation. Next, remember the entire discussion that we had between the frequency which means your respiratory rate and you multiply that by what? Your tidal volume. Which discussion, Dr. Raj? You remember, I gave you two big examples of increased respiratory rate and tidal volume being either low, what is that called, clinically? Good. Rapid shallow breathing. Example may be such as PE (pulmonary emboli) or number 2, rapid deep breathing. Give me example for that, that I gave you. Kussmaul breathing. What were the two parameters that we looked at? It’s tidal volume, respiratory rate. Of the two, which one was deep? Meaning, which one determined the depth of breathing? Good. The tidal volume. If you increase the tidal volume and increase the respiratory rate just a tad bit, you remember that alveolar ventilation? Isn’t that what you truly are trying to increase so that you have proper gas exchange? Is that clear? So, with that discussion, if you are unclear, make sure you go back to that discussion that we had when we specifically looked at alveolar ventilation, total ventilation, the frequency and then in terms of tidal volume. So tidal volume and respiratory rate, there it is, that is the frequency, to minimise barotrauma or volutrauma. You must. Next, some hypercarbia, what does that mean? Hypercapnia, same thing. And respiratory acidosis is actually acceptable. Is that clear? So, at some point in time, remember. At some point, you can’t introduce too much oxygen and you want to avoid barotrauma, so you call this permissive hypercapnia, especially in ARDS. In general, it’s okay to raise the respiratory rate, but tidal volume should be minimized. The formula for the recommended tidal volume is about 6 milliliter per kilogram of ideal body weight.
About the Lecture
The lecture Modes of Ventilation: Mechanical Ventilation Goals by Carlo Raj, MD is from the course Respiratory Failures.
Included Quiz Questions
What is a goal of mechanical ventilation?
- Minimize oxygen to avoid possible oxygen toxicity.
- Maximize oxygen to avoid possible oxygen toxicity.
- Increase the positive end-expiratory pressure to decrease airway trauma.
- Reach a PO2 of <60 mmHg.
Which of the following is the desired value of tidal volume during mechanical ventilation in patients with ARDS?
- ~6 mL/kg ideal body weight
- >6 mL/kg ideal body weight
- >7 mL/kg ideal body weight
- >8 mL/kg ideal body weight
- >10 mL/kg ideal body weight
Which of the following must be adjusted to maintain optimal minute ventilation?
- Respiratory rate and tidal volume.
- FiO2
- PEEP
- Peak pressure
- Plateau pressure
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |