Playlist
Show Playlist
Hide Playlist
Volvulus
-
Slides GIP Volvulus.pdf
-
Download Lecture Overview
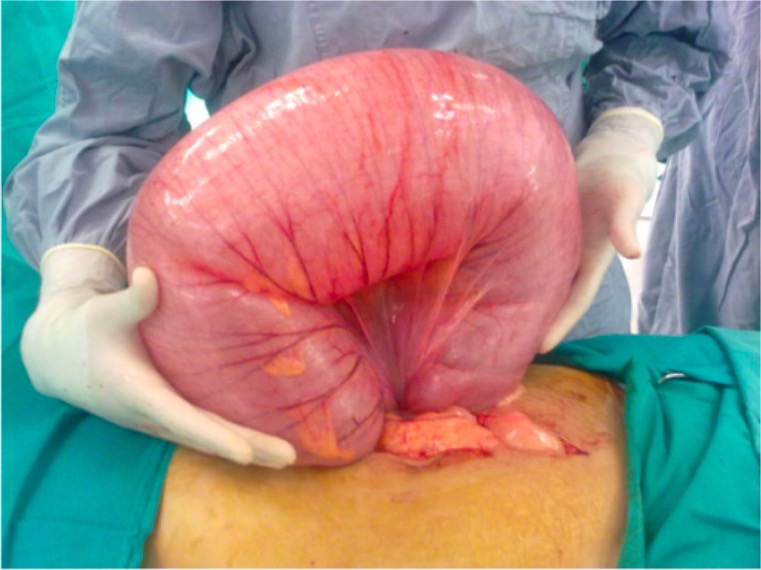
00:01 Welcome. In this talk, we're going to be covering an entity called volvulus. 00:06 You can think of this as being - as having your GI tract literally tied in a knot. It's the twisting of the bowel around its mesentery. 00:15 Now, in the talk that we're going to cover here, we're going to primarily focus on colonic volvulus but this can also clearly involve the other parts of the bowel, particularly, the small bowel. 00:29 And for example, with bowel malrotation, another talk in this series, we do talk a bit about volvulus involving the small bowel. 00:37 For here, keep in mind, this is going to be colonic volvulus. The epidemiology of this is that it's most commonly associated with surgery. 00:48 And when you have surgical intervention anywhere within the abdominal cavity, the manipulation of the bowel and putting in retractors and a little bit of fluid, a little bit of injury is going to give rise to a healing fibrosis. 01:00 That healing fibrosis may make tracts of fibrous connective tissue that go from one side of the peritoneum to the other side. 01:08 Those are adhesions and most of the time, in the vast majority of patients who've had prior surgery, nothing ever gets caught up in those. But the bowel is very motile and in some situations, it can be moving around and accidentally get caught up underneath a band of adhesion. 01:28 And when it does, that's where we're going to have volvulus. Overall, volvulus is the third most common cause of large bowel obstruction. 01:36 The most common causes are cancer and diverticulitis and we will cover both of those in a subsequent talk. 01:44 For colonic volvulus, the sigmoid is going to be the area most commonly involved. 01:51 The cecum is second. Transverse colon, relatively rarely and splenic flexure is the least common. 01:58 And again, just to tell you, the small bowel can also be tied up in knots and can be caused as well by adhesions. 02:09 So, sigmoid volvulus, the most common, typically occurs in older men, the mean age of 70 and in the vast majority of cases, there's been prior surgery. 02:18 It can sometimes affect, however, younger patients who have not had any surgery but have colonic dysmotility and there may be some torsion and twisting that happens with the normal or abnormal bowel movements. 02:33 Cecal volvulus on the other hand at the other end of the colon is more common in middle-aged women. 02:41 With regards to pathophysiology, we're looking here at your typical colon. 02:45 On the left-hand side is the cecum, ascending colon, hepatic flexure, transverse colon, splenic flexure, descending colon, sigmoid and into the rectum. Normal bowel activity will allow folding up. 03:03 I mean, the bowel is just squeezing, pushing things around. You may actually have loops that go up in the fashion indicated here. 03:10 If they happen to get caught underneath an adhesion or just to twist around on themselves, now, you have a volvulus. 03:18 And the problem is that in some cases, you can untie it. It just twists back the other way. 03:27 But in some other cases, it does not untie. As a result of that, the sequestered segments of bowel that are kind of looped out and captured have flora within them, they continue to make gas that causes increased intraluminal pressure. 03:43 The expansion of the lumen will then compromise the blood supply to that segment of the bowel, eventually, giving rise to ischemia and infarction and perforation. 03:55 And then, you're spewing bacteria and fecal contents into the peritoneal cavity. 04:00 The clinical presentation kind of makes sense once you understand the pathophysiology. 04:05 There is a gradual onset of pain and abdominal distension. The pain becomes constant. 04:11 And then, as the bowel tries to squeeze during its normal peristalsis, you may get periodic exacerbations. 04:19 With that pain and with the squeezing with the bowel distension, you may get nausea. 04:25 There's clearly constipation because you're not moving stool through the entire bowel and associated with the nausea, the re-vomiting. 04:33 The diagnosis is one of clinical history, prior surgery, the initial gradual onset of pain that becomes periodically worse. 04:43 And then, a physical exam that shows a distended abdomen and signs of peritonitis, especially, as we're getting closer and closer to perforation. 04:51 So, signs of peritonitis means that there is rebound tenderness. You press in, release, and it hurts. 04:58 Or there’ll be guarding the abdominal wall is very tense. That's associated with it. 05:04 Laboratories, depending on if there's infarction and other things, we will often see a leukocytosis, an elevated white cell count because there is infarction and inflammation. 05:15 The chemistries early on may reflect primarily a hypokalemic metabolic alkalosis due to vomiting of hydrochloric acid. 05:16 The chemistries early on may reflect primarily a hypokalemic metabolic alkalosis due to vomiting of hydrochloric acid. 05:18 The chemistries early on may reflect primarily a hypokalemic metabolic alkalosis due to vomiting of hydrochloric acid. 05:20 The chemistries early on may reflect primarily a hypokalemic metabolic alkalosis due to vomiting of hydrochloric acid. 05:24 On the other hand is we get to bowel infarction. Then we're going to see a metabolic acidosis with elevated lactic acid. 05:33 The imaging, you don't need to put him in a CT scanner to find this. 05:40 You can usually see the big, dilated loops of bowel without any contents in them on just a plain x-ray and that's what we're seeing here. 05:49 This is kind of the same thing now at surgery where you have a big dilated loop of bowel that has been twisted around its vascular pedicle and this part of the bowel has - will eventually become infarcted because the blood vessels will become compromised. The management, so, we would want to provide initial supportive management, fluids, correction of any electrolyte abnormalities, correction of acid and base balance. 06:19 We would hope that the bowel would twist back in the right direction and the volvulus would recede. 06:27 We can help that by making the patient NPO, nothing by mouth. We will do nasogastric decompressions, so, we'll put in a nasogastric tube and suction all gastric contents out. 06:39 And if we're getting - if we're worried about the possibility of ischemia or perforation, we'll give in to antibiotics. 06:45 Sigmoidoscopy from below may also release the pressure. And you may be able to treat the volvulus in that way. 06:54 But if we are not able to eliminate the twisting, we may actually have to go in and surgically resect the portion of bowel that is doing this, particularly, if there is now infarction and/or perforation. And with that, we've covered colonic volvulus.
About the Lecture
The lecture Volvulus by Richard Mitchell, MD, PhD is from the course Small and Large Intestines Disorders.
Included Quiz Questions
Which of the following is most commonly associated with volvulus?
- Prior surgery
- Cancer
- Inflammatory bowel disease
- Irritable bowel syndrome
- Hemorrhoids
What is the most common location of volvulus?
- Sigmoid colon
- Splenic flexure
- Transverse colon
- Cecal colon
- Rectum
Which is NOT part of the initial management of volvulus?
- Surgery
- IV fluids
- Electrolyte imbalance correction
- Nasogastric decompression
- IV antibiotics
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |