Playlist
Show Playlist
Hide Playlist
Eczema in Children
-
Slides Eczema Pediatrics.pdf
-
Download Lecture Overview
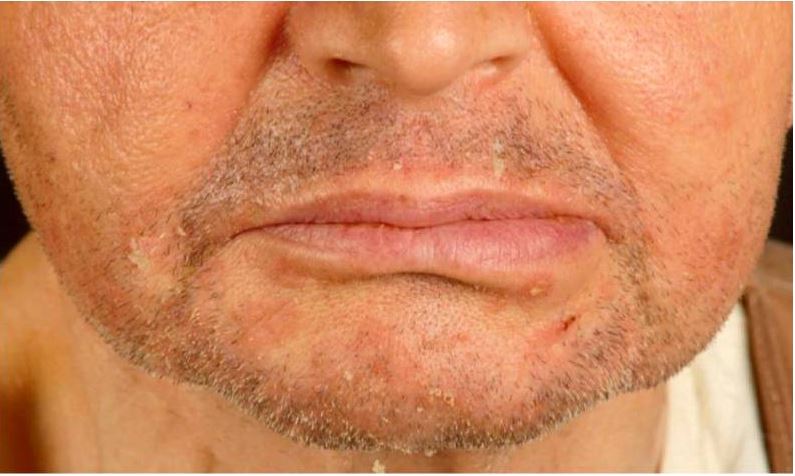
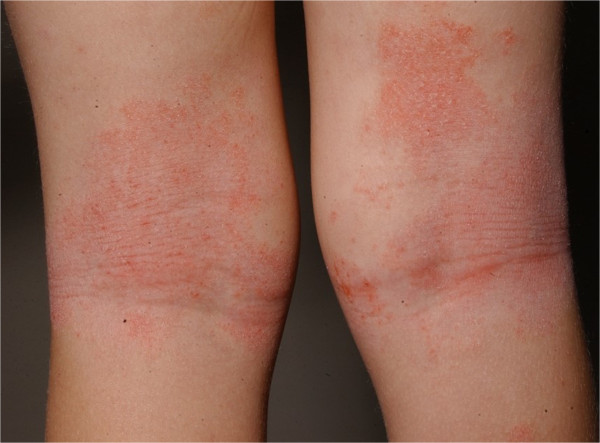
00:00 In this lecture we're going to discuss Eczema in Children, which is not only the rash that itches but also the itch that rashes because itching it is no good. This is a remarkable problem worldwide affecting between 5 and 20% of children and it involves both genetics and environment. So when you're encountering a patient where there is a history of potential eczema, you want to ask not only about family history but also about that child's history in terms of having both allergic disease, whether they have food allergy which is incredibly common in patients with eczema and up to a third and whether they have a history of asthma or wheezing that responds to albuterol, that's also incredibly common in these patients. So when you see eczema it's pretty easy to recognize it clinically. Here's a baby with pretty bad eczema. Eczema comes from the Greek which means "to boil over." It causes dry itchy papules and plaques on the skin with scale and crust and the clinical presentation varies by age but itchiness is fairly ubiquitous. So in infants under 2 years of age, it can present with itchy, red, scaly, crusty lesions generally on the extensor surfaces but also on the cheeks or on the scalp. 01:29 It typically spares the diaper area and is prone to bacterial superinfection. These kids can get bacterial cellulitis. Later in childhood between 2 and 12 years of age, there are fewer exudates less of that crusting weeping stuff and they start to develop lichenification. Lichenification, I'll show you a picture in a bit, is when it's been itching so much and it starts to thicken and they form plaques also on their flexural areas. In adulthood, it often becomes milder and maybe localized or lichenified. It can become excoriated, patients may have fibrotic papules and again it affects their flexural surfaces. So, remember location. At birth, we think of the face, the trunk and the extensor surfaces and in the older child we think of the flexural surfaces and areas where there might be friction. What we know about this disease is that it follows an itch-scratch-itch cycle so patients first become very itchy and they scratch at it. 02:42 That scratching of it exacerbates it and can lead them both to worse rash and the risk of infection. Here's a picture of lichenification. You can see these patients have been itching at their eczema for a while and it's forming that plaque-like surface. So the pathogenesis of the disease is that patients basically have some sort of epidermal dysfunction. They have a genetic deficiency of their skin barrier function, thus they have a robust TH2-mediated immune response to environmental antigens. Essentially, they are tucking their own skin with their immune system, they are failing to recognize self. This attack leads to an alteration of the skin microbiome which can in turn worsen the situation. These patients are at increased risk for cellulitis and that's one complication we have to worry about fairly frequently. Basically, they have broken down the barrier that is their skin and now they are itching it which can also help organisms get underneath the superficial skin layer. This is a bacterial superinfection. The treatment to prevent cellulitis is not only oral antibiotics but we will also have them do routine dilute bleach baths. These bleach baths will reduce the bacterial colonization of the skin. 04:13 Another complication of eczema is eczema herpeticum. This happens more commonly in young infants especially with their very first infection with the HSV virus, which is ubiquitous in all people, we're talking about HSV type 1 most typically. Children who have an underlying eczema are at increased risk for a variety of viral illnesses and this is unfortunately one of them. 04:41 Eczema herpeticum can be very severe. These patients may present with fever and it may be life threatening. Furthermore, if the area around the eyes is involved as in this patient, we need an ophthalmologist involved because it can be vision threatening as well. We treat these patients with IV acyclovir until they're improved and then they typically go home on oral acyclovir and we of course try to control their eczema. Clinical diagnosis of eczema is key. It's based on recognizing the rash that I've shown you in these pictures. You may see some lab findings like a total plasma IgE level that's elevated or eosinophilia but the reality is that is not something that we typically see and isn't very useful in the diagnosis. If the history of the patient suggests an allergic cause to the rash, we may do skin-prick testing or RAST testing to see if we can figure out what might be setting off their skin reaction. If patients have very severe or frequent infections of the skin, you might consider an immune-mediated problem. 05:54 They may have immunodeficiency in addition to their eczema. Examples of conditions like this include Job's syndrome which is a hyper-IgE and Wiskott-Aldrich. So let's think about the management of patients with eczema. The most important thing to do with all patients is to make sure their skin remains well hydrated with emollients. It doesn't really matter so much which emollient it is, it matters only that you're doing it routinely. We usually recommend patients use Eucerin or some other similar emollient at least twice a day. In patients with significant inflammation, we will use topical corticosteroids. Remember, topical corticosteroids come in various strengths. You can start with a low-strength topical corticosteroid such as 1% hydrocortisone and that's very useful especially for the face. Remember, higher-strength topical corticosteroids on the face can cause problems with discoloration; however, we will escalate the higher dose topical corticosteroids in patients with more significant eczema. 07:07 My general rule is if you're using a grade 4 or 5 steroid, you might think of involving a dermatologist. We also want to avoid, like I said, those high-potency steroids on the face. You really shouldn't be using those for a long time. We will provide antihistamines for itching in these patients, which is common. So Benadryl becomes a part of their life a little bit. In older kids you can use non-sedating antihistamines and again if patients have secondary infections we'll use antibiotics. We generally recommend loose clothing as tight clothing is more associated with disease and we sometimes, in little kids, suggest they just run around the house in their underwear because less clothing will confer less difficulty with the _____. 08:00 So that's my review of Eczema in Children. Thanks for your time.
About the Lecture
The lecture Eczema in Children by Brian Alverson, MD is from the course Pediatric Dermatology. It contains the following chapters:
- Eczema – The Itch That Rashes
- Secondary Skin Changes
Included Quiz Questions
All of the following are treatment options for eczema, EXCEPT?
- Tight clothing to stay warm in the winter
- Topical steroids
- Topical emollients
- Antihistamines
- Antibiotics for superinfections
Which of the following is an important risk factor for eczema?
- Family history of atopy
- Local trauma
- History of radiation exposure
- Air pollution
- Autoimmune disease
Which of the following clinical manifestations of eczema is more typically seen in children under 2 years of age?
- Involvement of extensor surfaces
- Lichenified plaques
- Less exudation of lesions
- Less frequent involvement of the face
- More localized disease
What is the usual location of rashes of eczema in older children?
- Flexor surfaces
- Extensor surfaces
- Lower limbs
- Face
- Genitalia
What is the most appropriate test to diagnose eczema?
- There is no specific test as the diagnosis is largely clinical.
- Skin biopsy
- Skin prick allergy testing
- Radioallergosorbent test
- Serum IgE level
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
4 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Great overview of the condition, symptoms in various age groups, and treatments.
I particularly liked the differences between the presentation at different ages.
I would review more of Brian Alversons lectures but I'm a bit time-poor. All his lectures on pediatrics are amazing. He communicates clearly and confidently
Does a great job summarizing the information, succinct, easy to understand. The oder in which the information is presented makes it easy to remember.